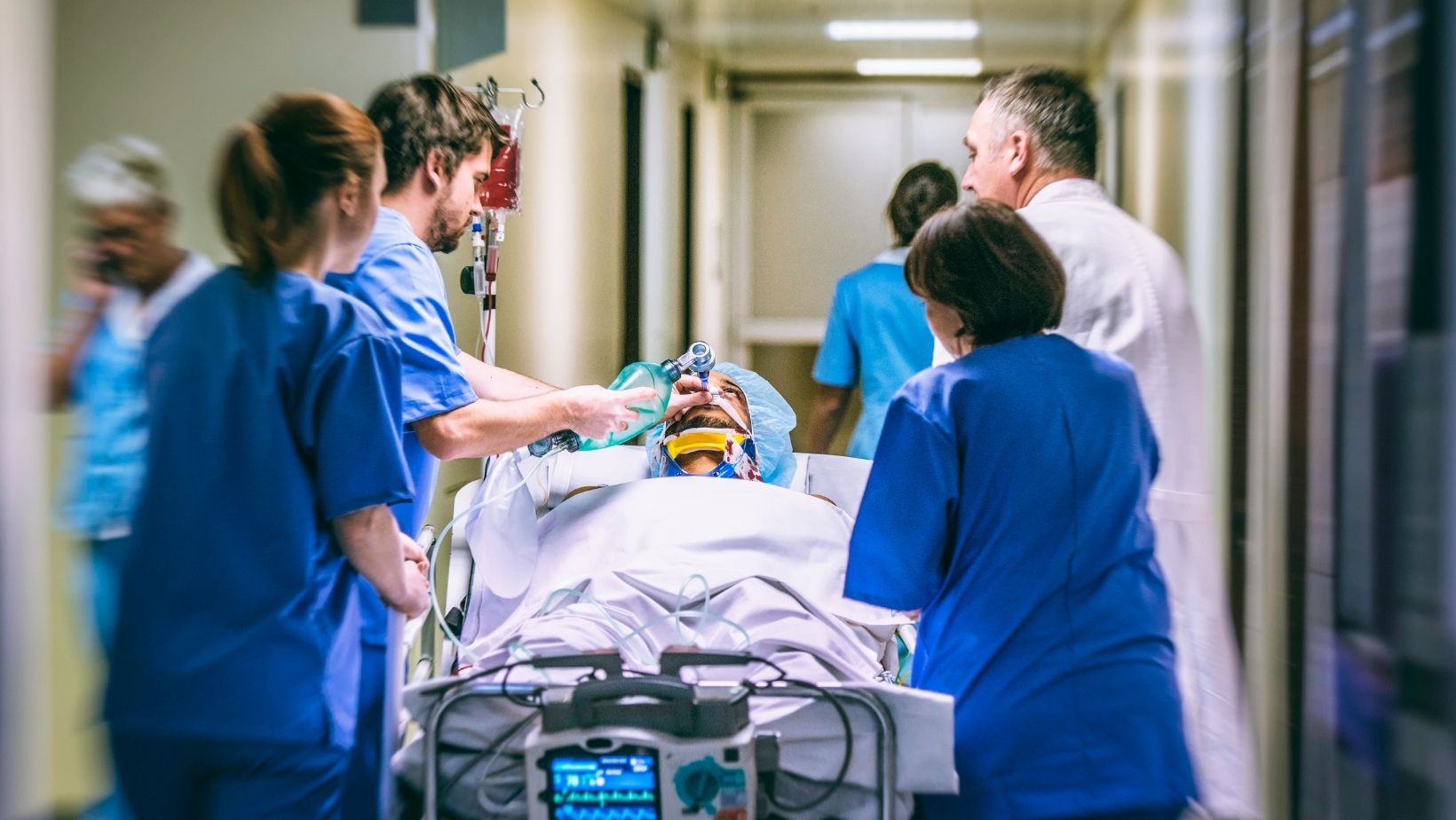
The emergency room is a high-pressure environment where every second counts toward a patient’s survival. It is a world defined by flashing lights, beeping monitors, and a constant stream of individuals facing the worst days of their lives. In this whirlwind, the atmosphere is often heavy with a sense of urgent necessity and clinical intensity.
To manage this volume, hospitals rely on a triage system designed to prioritize life-threatening cases over minor ailments. Nurses and physicians must make split-second decisions about who gets a bed immediately and who must wait in the lobby. This sorting process is the essential first line of defense in maintaining order within the medical facility.
However, when haste replaces clinical precision, the consequences can be devastating for a family. Doctors may overlook subtle symptoms of a major cardiovascular event while trying to clear a crowded waiting area. A fatal emergency room error regarding a heart attack or stroke can occur when the staff fails to listen to a patient’s specific complaints.
The Danger of Confirmation Bias in Crisis Medicine
One of the most dangerous psychological traps for a busy physician is known as confirmation bias. This occurs when a medical professional quickly settles on a diagnosis and then only looks for evidence that supports that initial theory. They stop considering alternative explanations for the patient’s pain, effectively closing their mind to other life-threatening possibilities during the evaluation.
For example, a middle-aged patient complaining of chest tightness and sweating might be dismissed as having simple indigestion or a panic attack. If the doctor assumes the issue is gastrointestinal, they might ignore the radiating arm pain that clearly points toward a cardiac crisis. This mental shortcut prevents the implementation of life-saving protocols at the most critical moment.
This bias is often fueled by the repetitive nature of seeing hundreds of patients with common, non-emergency symptoms every single week. When a doctor stops being an investigator and starts being a clerk, the quality of care drops significantly. Anchoring on a minor diagnosis while a major crisis unfolds is a hallmark of negligence in the ER.
Failure to Order Essential Diagnostic Testing
Diagnostic tests such as CT scans, MRIs, and comprehensive blood work are the objective tools that remove the guesswork from emergency medicine. These technologies allow doctors to see inside the body and identify hidden internal bleeding or early signs of organ failure. In a modern hospital, these resources should be the standard foundation for any serious medical evaluation.
Unfortunately, hospital overcrowding and aggressive cost-cutting measures often lead to a failure to order these essential tests. Administrators may pressure staff to limit the use of expensive imaging unless a patient meets a very narrow and specific set of criteria. This creates a dangerous environment where financial metrics are prioritized over the actual safety of the individual.
When a patient is sent home without proper imaging, the medical team is essentially gambling with that person’s life. A simple lab test might have revealed an infection or a chemical imbalance that could have been treated easily on-site. Skipping these steps to save time or money is a direct violation of the duty of care.
The Risks of Premature Discharge Malpractice
Discharge malpractice occurs when a hospital sends a patient home while they are still in a physically unstable or dangerous condition. The pressure to clear beds for new arrivals can lead to a rushed process where vital signs are not properly monitored before the exit. A patient might look fine for a moment, but their internal status may be rapidly deteriorating.
This premature release often results in the patient suffering a major medical setback shortly after they reach their own front door. Without the immediate support of hospital equipment and staff, a manageable complication can quickly turn into a fatal event. The trauma of being sent away while still in pain is a deeply disturbing experience for many.
Proper discharge requires a thorough review of the patient’s stability and a clear plan for follow-up care with a primary physician. When these protocols are ignored in favor of hospital efficiency, the facility is putting the community at unnecessary risk. Ensuring a patient is actually ready for the “real world” is a non-negotiable part of emergency medicine.
Navigating Immunity Laws with Specialized Counsel
Summarizing the risks reveals why victims of ER negligence need specialized legal counsel to navigate the complexities of their claim. Many hospitals are protected by “sovereign immunity” or specific “emergency immunity” laws that make it much harder to sue for medical errors. These statutes are designed to protect first responders but can often be used as a shield against accountability.
An experienced attorney knows how to peel back these legal layers and identify the specific failures that led to the harm. They work with independent medical experts to recreate the timeline of the ER visit and prove where the system broke down. This professional investigation is the only way to overcome the high hurdles set by state laws.
Ultimately, seeking justice for a misdiagnosis is about demanding a higher level of care for every patient who enters a hospital. By holding negligent parties responsible, families can secure the resources needed for their recovery and long-term health. A focused legal strategy ensures that the “chaos” of the ER is never an excuse for a lack of precision.



